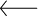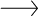While she was carrying her third child, Tanisha Fuller had to convince her hospital caretakers that something was really wrong. It was 2003, she was six months pregnant, and she was unsure of what was happening to her. The Richmond resident had rushed to the emergency room at Alta Bates hospital in Berkeley with pain in her back, feeling like she couldn’t breathe. At the hospital, she was told that it was “probably gas,” she said, given a Tylenol, and told to lie down in the examination room.
She asked for an X-ray. Looking back, she isn’t sure why. “It had to be God,” she said.

Kiko Malin said it’s important to consider the “social factors that might be driving” the disparities between racial groups apparent in the health department’s data. Credits: Photo by Drew Costley 
Tanisha Fuller said her son, L.C. Fuller, is now “the tallest and biggest out of all my kids, which is crazy.” Credits: Photo courtesy of Tanisha Fuller
“They did it, and came rushing out,” Fuller said. Someone told her, “‘Your lung collapsed. Let’s get you into surgery.'” The medical staff placed a breathing tube in her chest; she ended up needing to use one until she delivered.
At the time, nobody told her that the complications from her lung meant her baby was in danger of being born “preterm” — before 37 weeks of pregnancy had been completed. She just knew that she needed to get to three different appointments each week: one with a high-risk doctor, one with a pulmonologist, and one for a stress test. Though she had two other kids at home — ages 6 and 1 — was working, and didn’t have a car, Fuller didn’t miss a single appointment.
At one of her weekly stress tests — during which “you go lay down for 30 minutes and they hook the baby up to a monitor that makes sure it’s not in distress,” she said — Fuller learned that her baby was, in fact, in distress. He wasn’t “responding well to everything that was going on,” she recalled. The medical staff feared that, if another complication with Fuller’s lung arose, it might affect both mother and child.
Fuller’s health care providers decided she needed to be induced — to have her labor started early. “I was scared. I was terrified. I was crying, because I just didn’t know,” she remembered. “I didn’t know if that meant that my baby was not going to make it. I didn’t know if it meant there was something wrong with me, and I was going to die.”
After a couple of hours at Alta Bates, a nurse finally explained that Fuller’s team of health care providers felt that inducing her was the safer option and told her what would happen.
A few days later, Fuller went home with a 5-pound baby — her son came just short of a month early. Everyone at home was scared to touch him because “he was so tiny,” she said. “I had to kind of learn on my own how to take care of him.”
For women in the United States, giving birth to a preterm baby is a fairly common experience. The Centers for Disease Control reported that, in 2016, “preterm birth affected about one out of every 10 infants born in the United States.” Babies who are born too early, according to the CDC, “have higher rates of death and disability.” They haven’t yet fully developed, and it’s harder for them to adjust from life inside their mothers to functioning on only their own bodies’ systems.
[pullquote-1]As widespread as this problem is, it’s more prevalent for some mothers than others. Nationally, the rate of preterm birth among African-American women, like Tanisha Fuller, was about 50 percent higher than that experienced by white women in 2016, according to the CDC. Even in the affluent Bay Area, between 2012 and 2014, African-American women were almost twice as likely to give birth to preterm babies as women of other races, according to data published by the Alameda County Public Health Department last year.
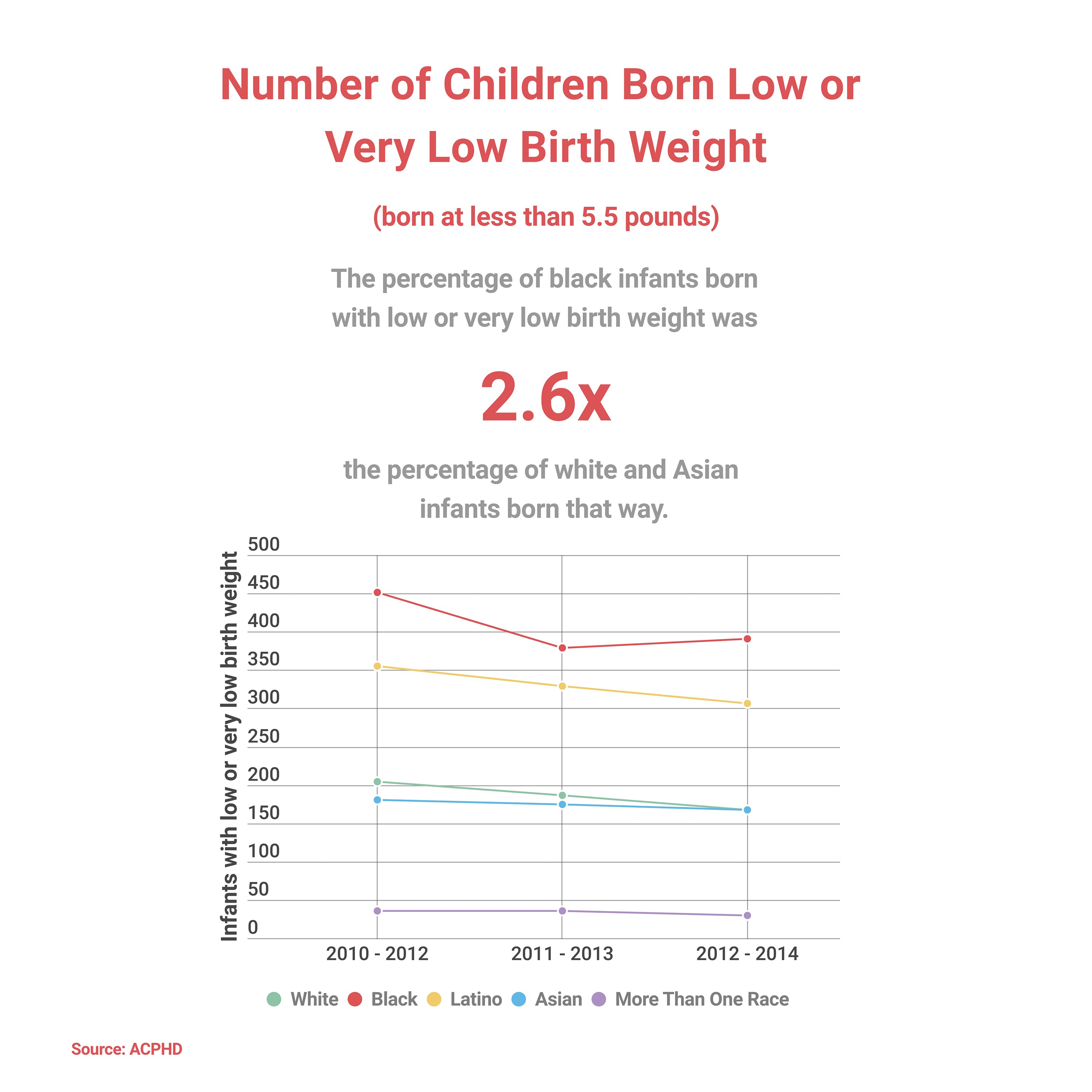
According to this same data, Black women in the East Bay are also nearly three times as likely to give birth to low birth weight babies — infants born weighing less than 5.5 pounds — than are white women. Babies born this small are “approximately 20 times more likely to die than heavier babies,” according to a 2004 report by the World Health Organization.
Although African-American babies were only 9.8 percent of the total births in Alameda County between 2012 and 2014, they made up more than a quarter of the infant deaths during that time. They are also more than four times as likely as white infants to die from disorders related to being born with a low birth weight or to having a gestation that was too short, as well as from causes like Sudden Infant Death Syndrome (SIDS).

Maternal mortality, though it affects a very small number of women in California, also disproportionately affects African-American women. In 2013, according to data compiled by the California Health Care Foundation, about 26 of every 100,000 pregnant Black women died —almost four times as many as white women, who died at a rate of seven per 100,000 that year.
“We know that African Americans are more likely to have a preterm birth, more likely to have infant mortality,” said Allison Bryant, a Boston-based physician who is a member of the American Congress of Obstetricians and Gynecologists’ Alliance for Innovation on Maternal Health. As a result, she said, Black families probably carry a disproportionate burden due to the health consequences of preterm birth.
Babies born too small or too early, Bryant said, often need to stay in the hospital nursery or in the Neonatal Intensive Care Unit (NICU) “for a long period of time.” After leaving the hospital, they tend to have chronic health challenges, which means more provider visits, equipment, and monitoring.
“Sometimes, babies go home with an apnea monitor to make sure that they are not stopping breathing at particular instances. Some babies have retinopathy of prematurity, which is an eye disease, which then probably needs more ongoing care and attention. They have chronic lung disease, which then means more doctors’ visits and perhaps oxygen,” said Bryant. All of the complications of prematurity “are going to be borne more heavily in the communities that are more affected by preterm birth.”
Early birth can also lead to developmental or learning issues later in childhood. “Babies who are preterm, or babies who are born very low birth weight,” Bryant said, “are less likely to gain a high school diploma or a GED, [and] they have more behavioral issues.”
Though overall rates of infant mortality, preterm births, and low-birth-weight births declined in Alameda County between 2000 and 2014, the racial inequities persist. Local groups like the Preterm Birth Initiative and Black Women Birthing Justice are working to learn more about the risks and challenges women of color face within the health system and to educate women about their options and rights. But because these problems don’t have just one cause, many feel that changes to improve the health of women and infants will be incremental.
“There’s no smoking gun. There’s no one thing that you could fix that would then drive the preterm birth rates down by half,” said Bryant. “Every little bit helps.”
These inequities are a problem for all Americans, said Monica McLemore, a registered nurse in Oakland, “because we are robbed of the brilliance of everyone’s children and the perspectives of those children and the gifts and talents of both them and their parents.”
Sommer Davis wanted to be a labor and delivery nurse since she was 7 years old. She never dreamed of a fancy wedding, only of giving birth and being involved in others’ births. “I was trying to describe to my daughter the other day, what it’s like,” Davis said. “She says she wants to be a nurse, too. So, I said, ‘If you help the mamas with their babies, you get to be a part of the most overwhelming experience of love in a stranger’s life every single day.'”
Lean and tall, Davis is warm and attentive to the comfort of those around her. This quality has probably only become stronger during her 15 years as a labor and delivery nurse, the last two and a half spent at a hospital in Alameda County. (Davis declined to name the hospital where she works because, she said, employees aren’t allowed to represent the organization’s views.)
Davis said she sees one to three cases of either preterm birth, low birth weight birth, or infant mortality on a daily basis.
Depending on the “gestational age and overall well-being” of the baby, Davis said, there are a variety of ways the nursing staff can care for a preterm infant. “Often, extreme premature babies will not eat for several weeks and their nourishment is taken care of via IV,” Davis said.
Hospitals use warming pads for extremely premature babies, because they don’t yet have adipose tissue — connective tissue made up mostly of fat — under their skin that would regulate their temperature. Breathing machines are used for babies whose respiratory systems aren’t yet adequate or who have some other breathing issue.
For babies born too early or too small, Davis said, “breastfeeding issues are common.” She added that these situations “could possibly delay healing of the mother due to stress and also place her at higher risk for postpartum depression.”
[pullquote-2]In some cases, preterm births happen through induction, but Davis said that doctors would only elect to induce labor before 37 weeks if the baby or mother were facing a serious illness or complications, as in Tanisha Fuller’s experience.
The induction process can take days to cause active labor, as physicians run through what Davis calls their “induction toolbox.” It can be long, exhausting, and painful for the woman. She might need to wear an external fetal heart rate monitor — a strap that goes around her belly and monitors the baby’s heart rate — or in some cases an internal monitor that’s placed through the vagina. She may have a Cook Balloon placed in her cervix to manually dilate it. (“It’s these two water balloons that go in the cervix and sort of squash the cervix,” Davis said, “and you can leave it in for up to twelve hours.”) She may receive Misoprostol, a drug that can cause minor uterine contractions, or Pitocin, a synthetic version of the hormone oxytocin — which, Davis said, is essential for causing contractions — or both of these.
By the time a woman has to push her baby out, she’s often sleep-deprived and dealing with a lot of pain while in that state. Then more interventions — intravenous pain meds, epidurals — can happen to get her through the birth.
While Davis is glad to help mothers through all of these situations, she wishes she could do more. “I often think about what it’s going to be like for them when they’re discharged home. The physical recovery, I think, is challenging,” Davis said, “but it’s always the emotional scars that take a longer-lasting toll.”

She worries, too, about the babies. “Extremely premature infants often will have disabilities in their life — developmental, hearing, vision, speech,” she said. These struggles, “coupled with a challenging socioeconomic situation in the family, can lead to a very challenging life for both the growing child and its parents.”
Dr. Bryant said it would be very difficult to point to a specific cause for any particular preterm birth because there are so many factors involved in each case. There are, however, things that make preterm birth statistically more likely: if the mother has an infection, for instance, or if she smokes.
Other risk factors, according to Bryant, are “maternal diseases, fetal abnormalities, multiple gestations [carrying twins or triplets], and uterine abnormalities.” All of these things, and more, she said, “are statistically associated with an increased risk of preterm birth, but are not necessarily” the cause.
Christina “Kiko” Malin, family health services director at the Alameda County Public Health Department, said it’s important to consider the “social factors that might be driving” the disparities between racial groups apparent in the health department’s data.
Malin said African Americans are more likely to live in low-income neighborhoods. She also pointed to the issue of “fragmentation of care,” meaning women not getting continuous care because something changes with their provider or their insurance, or they lose their coverage altogether. This is most likely to happen to a low-income family, in which the parents may not have steady insurance through an employer. In these cases, a woman might not get the regular care she needs, or her providers might not be able to communicate effectively about her care.
Some women who are “increasingly marginalized” and “very stressed” may have a hard time keeping appointments, Malin said. “For folks who have to choose between putting food on the table or getting kids to school, a medical appointment might not seem as high of a priority, so the care is not as coordinated, as thorough, as it probably could be.”
For low-income women, part of the problem starts long before pregnancy. “We spend a ton of money on medical care and relatively less on social programs,” said Bryant.
The poor health outcomes for women of color, Bryant said, are partly due to what she called “the social determinants of health” or the hardships they suffer outside of the medical system, and which might hinder them from getting the care they need. “Do they have transportation issues? Do they have issues with childcare? Do they have food and security? Do they have housing issues? Do they have issues with the legal system?” Bryant said. “We care for our patients for a small slice of their life, and so it’s a little crazy that we think everyone’s health outcomes are so dependent on the care that they receive, when really so much of their health outcomes have to do with the milieu in which they live and work.”
These struggles aren’t unique to African Americans, but, Bryant said, they disproportionately affect her patients of color, who bring all of those issues “with them in terms of their health and healthcare.”



According to the Child Health USA 2013 report, produced by the U.S. Health Resources & Services Administration (HRSA), nearly 20 percent of mothers between 2009 and 2010 reporting from 30 U.S. states weren’t able to access prenatal care as early in their pregnancies as they wanted to. Nearly 23 percent of non-Hispanic Black mothers reported delayed access to care, as compared with 14.7 percent of white mothers.
“Common barriers to getting prenatal care as early as desired [or at all],” according to the report, include a lack of money or insurance to pay for visits, issues with transportation, and “not knowing that one is pregnant.”
While African Americans face the widest gap in infant health outcomes, other groups in Alameda County face similar disparities. For instance, from 2012 to 2014, while the Hispanic and Latino population experienced the lowest percentage of premature births, they represented more than a quarter of the infant deaths in that period.
Angelica Foreman, a Berkeley resident who identifies as Latina and whose husband is African American, went into premature labor with two of her three children. She went into labor with her first son when she was around 7 months pregnant, and her doctor placed her on bed rest. She carried him to term and was able to “deliver naturally,” she said.
[pullquote-3]Her next pregnancy was more eventful. Foreman went into labor at 30 weeks and was immediately admitted to Kaiser Oakland. Her medical providers wanted her to stay so they could observe her, and so that she would be there should her labor progress. When she went into active labor in her 32nd week, her baby’s blood pressure dipped. Before long, her blood pressure was dropping, too. When her son’s heartbeat was no longer registering on the monitor, hospital staff told Foreman they had to deliver him.
“I was flooded by, like, 15 doctors,” Foreman recalled. “They came in the room, they lifted me up, put me on the gurney, and they were, like, shooting me down the hallway so fast.”
Her son was delivered via C-section. Foreman said she had adverse reactions to medications during the surgery and an infection afterward. Much of the experience was “terrifying,” she remembered.
Her son was in the NICU for two and a half weeks. Though he was breathing fine, he had trouble eating because he hadn’t yet developed his sucking reflex, Foreman said.
According to Dr. Amanda Williams Calhoun, physician maternity director at Kaiser Oakland, the most common problems for preterm babies during their first month of life are with breathing and digestion.
In early childhood, “the risks are around chronic lung disease, asthma, some learning difficulty, cerebral palsy” and vision problems, Calhoun said. In general, most of these problems resolve as children grow into adults.
Today, Foreman and her two pre-term sons, now ages 6 and 19 months, are healthy. “This kid is off the charts,” Foreman said of her second son. “With weight, with height — he’s been pretty amazing, actually.”
In the Bay Area, two groups are trying to understand why these disparate health outcomes exist, to help mothers understand the resources available to them and teach them how to advocate for themselves. A third is working to address the social determinants that affect mothers’ health.
The Preterm Birth Initiative, a UC San Francisco program that brings together researchers from disciplines across the university, has been holding focus groups in San Francisco, Oakland, and Fresno. With these groups, the researchers were “really trying to get at, what are women’s experiences of their care,” said Oakland nurse Monica McLemore, a principal investigator for the initiative. They wanted to know what questions mothers had when they were pregnant “that were never answered or that they really wanted to be able to ask,” she said.
During her work with the Preterm Birth Initiative, McLemore heard from African-American women about interactions with health care providers who were disrespectful, neglectful, or didn’t believe their patients — things, she said, “that we probably would not accept in any other domain of health services provision.”
Because the paper about these focus groups is under peer review, McLemore didn’t feel comfortable discussing specific examples of the issues mentioned above, but said that, generally, the neglect and disrespect manifested themselves in situations such as mothers “having birth plans and having them be ignored,” hospital staff “policing who could and could not be with laboring people,” and a “disregard for symptoms — when people say epidurals aren’t working or something just doesn’t feel right.”
McLemore thinks that part of this problem stems from a lack of coordinated care by health care providers — part of what Malin called the “fragmentation of care.” McLemore said that, “to ask pregnant people to navigate those discordant systems is also really problematic.”
Add to these negative experiences an automatic assumption by some providers that their African- American patients are high-risk, “when they may or may not be,” said McLemore, “because there are still clinicians who actually believe that it is the Black race that is exclusively associated with these poor outcomes,” said McLemore. “Race only overexposes you to racism, but there is nothing inherent about black skin that makes pregnancy any more dangerous than it is for any other pregnant person.” This assumption sometimes means that Black pregnant women undergo unwanted procedures or tests, McLemore said.
In an effort to provide respectful care, McLemore listens to her patients and doesn’t assume authority over them, she said. “First of all, I start from a place of not believing I know everything, despite the fact that I have tons of degrees and I’ve been a nurse in women’s health for 26 years, mostly all focused on reproductive health. I walk into my clinical care environment trying to determine what are my patients supposed to teach me that day,” she said.
Like many health experts, she strives for “cultural competency” — not only literally speaking the patients’ language but creating space for the patients themselves in making decisions about their care. “It is about an intentional effort to understand where women are coming from when they come in the door of your health care system or your clinic,” said Bryant, who endorses similar goals.
[pullquote-4]Another group, called Black Women Birthing Justice, is working to educate women about their options when pregnant and giving birth. Based in Oakland, the collective of academic researchers, midwives, doulas, breastfeeding educators, and students put out a report in October called “Battling Over Birth,” which included suggestions for improvements in the health care system and birth stories collected from Black mothers around California.
From 2011 to 2015, members of the group and a team of co-researchers collected narratives and questionnaires from 100 Black women who gave birth in 11 California cities and towns. The women included in the small study were 17 to 46 years old. Each woman — cited only by first name — shared her experiences with giving birth either at a hospital or at home assisted by a midwife or doula.
The researchers found that, for the women they surveyed, the health care system itself was a source of stress. A woman named Zanthia, who birthed four of her eight children before she turned 20 and used the health care system in Oakland for two decades, told the researchers that she had many negative experiences within the system, but that prenatal care was the worst. At her prenatal visits, she felt routinely disrespected and, as a result, stopped going. “They would talk about me,” she said. She recalled nurses pushing birth control on her — “not even the kind I’m scheduled for” — and that she had doctors tell her, “Just go ahead and get an abortion.”

But the women also told stories of stressors in everyday life. Dalia told of moving out of her home in Oakland after a stray bullet landed on her family’s piano. She and her husband wanted to have another child and realized the place that was supposed to be their “safe space” couldn’t be that.
A mother named Dana recalled a harrowing year spent in and out of jail, during which she also endured the loss of her father, the murder of a brother who was “shot 34 times,” and the loss of her baby when she was two months pregnant.
Chinyere Oparah, a professor at Mills College and co-founder of Black Women Birthing Justice, said it’s important to acknowledge the disparities in health outcomes for Black mothers but cautioned against what she called the “culture of fear.” “Yes, Black women in California are four times more likely to die,” she said, referring to the California Health Care Foundation data, released in 2016. “However, most Black women are not going to die,” Oparah added.
“It is an incredibly uncommon thing to have a mother die,” agreed Calhoun, who’s been at Kaiser Oakland for 13 years. During that time, she said, about 28,000 babies were born at that hospital and there has been only one maternal death. (The woman who died was not African American, she added.)
Still, Oparah said, half of the women who participated in the Black Women Birthing Justice study recalled their time at the hospital as a frightening experience. They “were terrified, not only of the pain but of the possibility of death or that the baby might die or be disabled,” she said. “We even had participants talking about the kinds of statements that were made by nurses and physicians in full knowledge of that fear, saying things like, ‘Well, you don’t want a dead baby, do you?'”
In addition to researching and writing their report, members of Black Women Birthing Justice have worked to raise awareness of these inequities through social media and blogging; trained 16 women to become doulas (who have since formed a group of their own, the Roots of Labor Birth Collective); and edited a book, Birthing Justice, which includes “critical analysis to get people to really understand what the whole scope of birth justice was about,” said Oparah.
They also wrote a chapter about the research methods they used for the study for Research Justice, a book edited by Andrew Jolivette. “Research justice is a way of recognizing that research has historically undermined and disempowered communities of color. Oftentimes, we’ve been the victims of research rather than the beneficiaries,” said Oparah. “To change those power dynamics, research justice puts research tools into the hands of community members so that we can then develop community-driven research where we actually decide the research agenda, how the research should be conducted, how you analyze the findings, and what you should do with them in terms of action.”
Oparah believes improving maternal health outcomes is part of a broader push to improve the lives of people of color. “We should be looking at not just the streets and the police and the prison system and how Black people are losing their lives there, but actually we should be looking within our maternal healthcare system and the unnecessary deaths happening there both for Black women and infants,” she said.
[pullquote-5]While the Preterm Birth Initiative and Black Women Birthing Justice focus on birth and women’s experiences with health care, a third group, the Best Babies Zone Initiative (BBZ), is trying to provide social support and alleviate inequities among women before they actually get pregnant. “Our work is really focused on the social determinants of health,” said Mariela Uribe, program manager for the initiative’s Oakland site.
BBZ Oakland, which has been working since 2012, focuses on the East Oakland neighborhood surrounding Castlemont High School because, Uribe said, “data told us that there were clearly some birth inequities there.”
The initiative’s work is different every day, Uribe said, but at the core, they focus on using “community leadership and resident engagement” to connect “people to traditional health services” and encourage economic development.
A couple of the initiative’s key projects, said Uribe, are the community market they host in East Oakland during which “local entrepreneurs get to showcase their talent” and test-sell their products. “We have community health outreach workers going out and referring people to case management programs and connecting them to resources, when needed,” she said.
Who is in leadership is important. McLemore, of the Preterm Birth Initiative, said the lack of diversity in the health care profession needs to change, and the poor outcomes faced by African-American women are related to “a real inability for us to diversify our workforce.”
Calhoun, of Kaiser Oakland, echoed this concern, saying that there’s data showing that “patients will hear you differently if you are of a similar race or ethnicity.” Patients taking the advice, and feeling heard in return, “is associated with better outcomes,” she said.
Calhoun said her hospital tries to intentionally recruit doctors that can best support their patients, 25 percent of whom, she said, are Black. “As an African-American physician, myself, I’ve heard anecdotally countless stories from patients about how they felt listened to differently,” said Calhoun. “Did they get the right prescriptions? Sure. Did they get the right admission or non-admission to the hospital? Sure. But that experience of being listened to by your doctor and respected by your doctor is really where it makes a difference on the margin. Not the big data outcomes, but really at the edges.”


McLemore believes barriers should be removed for Black people wishing to enter health care professions. “People perceive that as a lowering of standards, but I argue it’s not true. GRE scores don’t correlate with success in graduate school,” said McLemore. “We also need to make sure people with criminal histories or justice involvement are not barred from seeking employment in the health professions.”
McLemore is hopeful that “this call for more respectful, holistic care is something that will trickle through health care,” but, she said, there will need to be some financial incentive, “as long as health care is continuing to be moved and motivated by those things.”
The Preterm Birth Initiative is planning to make information about their focus groups publicly available, “similar to the Black Women Birthing Justice report,” said McLemore. The initiative is also working to create an app that would offer answers to the kind of questions raised during their focus groups. They might even launch a YouTube channel for this purpose. Their goal is to make “tools that aren’t just in the scientific literature, so that we can get this information out to people,” McLemore said.
For Tanisha Fuller, part of the solution is sharing her own birth story with other women. She now lives in Antioch, and her son is 13 years old and healthy. Even though he’s her youngest, Fuller said, “He’s actually the tallest and biggest out of all my kids, which is crazy.”
At her office building in Oakland in the summer of 2016, Fuller got to talking with the women who were holding a Preterm Birth Initiative focus group in the building’s conference room. She soon found out that they were one person short. She joined the women who, while waiting for the talk to begin, were chatting about doulas. Doulas don’t deliver the baby or offer medical treatment. Their role is to provide support where the birthing parents need it — this can be anything from grocery shopping to cleaning up the house to massaging the mother during birth.
After her own son’s birth, Fuller had started trying to answer friends’ and family members’ questions about birth complications. “I’ve always been there when it comes to them having a baby or being pregnant. I just shared the knowledge. I was being a doula already, but I just didn’t know it,” she said.
When she found out that doulas play a similar role — “basically, being a support system for the birthing parents,” she said — she was eager to learn more. The women from the initiative encouraged her to pursue that path, even offering to pay for her training.
That fall, Fuller completed her training over two weekends at a midwife’s home in Oakland. She learned about the female body and how it functions during and after pregnancy. She learned how to support a woman during her labor by reminding her of, say, the reasons why she had chosen not to have an epidural. She learned how to help the woman’s partner get involved during the birth: “You’re there to say, ‘Hey, why don’t you come rub her back?’ or ‘Hey, why don’t you guys dance?’ — something like that to get them involved.”
Thanks to her own three births, including her frightening experience with the preterm birth of her son, she knows how isolating it can feel to go through something really difficult and unfamiliar. “I can sympathize. I know how it feels,” Fuller said. “That’s what makes me want to do this, because of my experience and wanting to help someone else.”
After having been a doula for a year, Fuller said, she wants to tell women: “You do not have to do this by yourself.”
A version of this report was originally published by Oakland North, a project of the UC Berkeley Graduate School of Journalism.Written by Sarah Hoenicke with additional reporting from Drew Costley and Sarah Cahlan. Videos by Sarah Cahlan and Drew Costley with production assistance from Sarah Hoenicke and Anne Wernikoff and illustrations by Suzanna Hoenicke.